“This is the first hospital I’ve been to that has welcomed me like this.”
Your support will help patients like Enoc access dignified care for tuberculosis and other infectious diseases.

SBH’s tuberculosis tent is tucked away on the far side of the hospital campus, near a cholera tent but visibly more isolated. Before patients and staff enter, they are required to put face masks on, so as to prevent transmission of the highly contagious bacterial infection.
Walking up toward the tent can be fairly intimidating because prevention protocol is taken seriously, but today the inside of the tent is unexpectedly lively. Patients are sick, but in good spirits—chatting from behind masks, some even eating lunch from the hospital cafeteria.
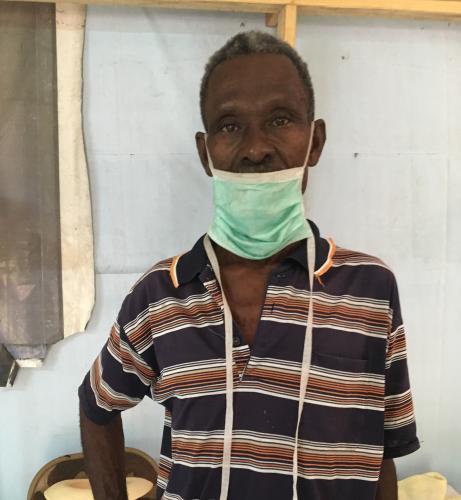
SBH has recently seen a small upswing in tuberculosis cases. In the past month, we have had more TB patients than in any other month of 2016; seven are currently being treated. One of those patients is 68-year-old Makoel Biduet—a farmer from Ferdile, a rural town east of Fond des Blancs.
Makoel, a father of eight, came down with flu-like symptoms three weeks ago which left him bedridden in the home he shares with his large family. His wife summoned a nurse who lives in the community to check on her husband, who, at that time, was suffering from a sore throat, cough, and fever. The nurse prescribed Makoel cold medicine, but the treatment didn’t seem to be helping.
“I am the only person who works in my family, so until I was very ill, I worked the fields,” he says.” But eventually, my symptoms became so severe that I couldn’t do much manual labor anymore. I prayed that the nurse would be able to help me, but it became clear that my illness wasn’t just a common cold.”
After several agonizing days, his condition became dire. Makoel took a five-hour moto-taxi ride to SBH—the closest treatment center. But he didn’t expect that he’d be staying here quarantined for the next fifteen days.
I didn’t even know what TB was. But I could tell from the doctor’s face that it was serious,” he recalls.” Then I was told I’d have to sleep here and miss many days of work—which I didn’t want to do. But the staff made me see how dangerous the disease is, so I agreed.
Maokel
Makoel immediately began a serious regiment of treatments, which includes four different medications to be taken daily. He was dispatched from the hospital today and is no longer contagious. He will continue taking medication for the next six months. Otherwise, his infection could return—potentially deadlier than before.

As our community health director, Miss Yanick, knows all too well, the biggest challenge in treating TB is holding patients accountable for their own treatment.
“It’s difficult to make sure that patients who don’t live in the area are taking their medication,” says Miss Yanick. “Also there’s a huge stigma about the illness. Often, the community and family members don’t support TB patients through the course of their treatment and beyond; patients tend to feel very isolated.”
Miss Yanick finds that misinformation is also detrimental to the treatment of TB in Haiti, so she is sure to be very specific in explaining to patients how and when to take their medications.
“Many people here think that medication must always be taken with food, but that’s not the case with TB medicine. Sometimes patients won’t take their meds because they don’t have any food to eat, even though taking it with food isn’t necessary,” she explains. “In other cases, people discontinue treatment before six months—once they start gaining weight and feeling better. And often, they will become sick again.”
Makoel will return for a follow-up appointment in two weeks to make sure his condition is improving and he is staying on top of his treatment.
“Everyone at St. Boniface has been so good to me. I get hot meals here, which I sometimes go without at home,” he says. “If I could change one thing about my experience here, it would be staying in this hot tent. Being in a ventilated building would have made the healing process much easier.”
Little does Makoel know, his wish is coming true for future patients. Our construction partners at Build Health International have started rendering plans for SBH’s new Infectious Disease Center, expected to open in 2017. The building will be constructed on a plot next to the isolation tents and will make it so patients can be treated in comfort but still separated from the main ward to prevent infections like TB from spreading.
Your support will help patients like Enoc access dignified care for tuberculosis and other infectious diseases.
